Last Updated: April 2026
Introduction
CPT code 90834 is the most commonly used psychotherapy billing code in behavioral health medical billing in the USA. At UtreatiBill, we maintain a 96% clean claim rate for CPT 90834 psychotherapy claims, based on internal billing data across Medicaid and commercial payers. This significantly reduces denials related to eligibility, modifiers, and documentation errors.
This guide is built on those numbers. Not theory.
What Is CPT Code 90834? (45-Minute Psychotherapy Billing Explained)
CPT code 90834 = Psychotherapy, 45 minutes with patient and/or family member face-to-face.
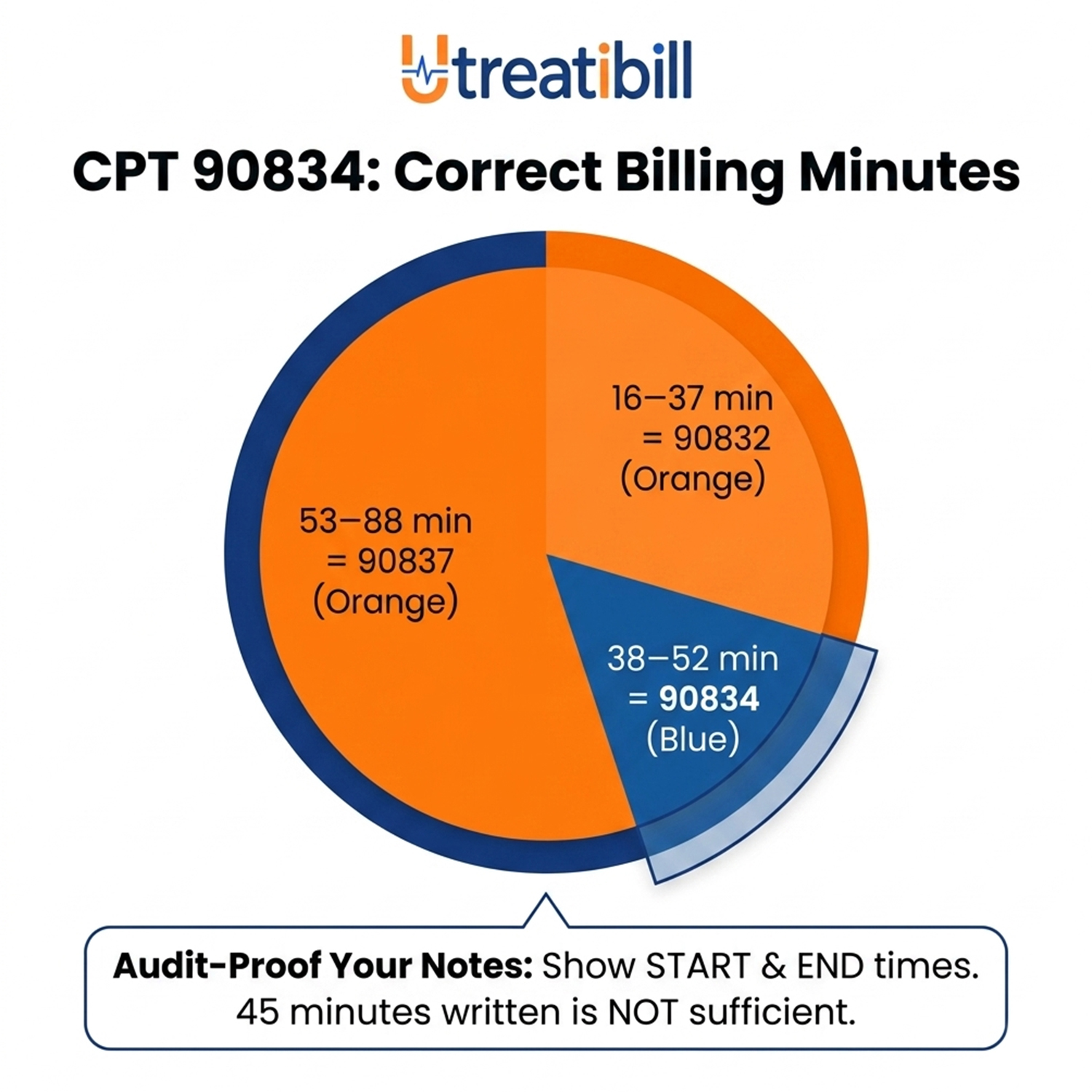
CPT 90834 time range (CMS official guidelines): 38–52 minutes.
| Minutes Billed | Correct Code |
| 16–37 | 90832 |
| 38–52 | 90834 |
| 53–88 | 90837 |
90834 documentation requirements are strict. Payers audit time stamps. Your note must show start and end time. “45 minutes” written in a text box is not sufficient.
CPT 90834 vs. 90837 vs. 90832 (2025 Reimbursement)
| Code | Time | Commercial (Avg) | Medicaid (Avg) |
| 90832 | 30 min | $62 | $38 |
| 90834 | 45 min | $98 | $72 |
| 90837 | 60 min | $125 | $88 |
90834 reimbursement rate 2025 varies significantly by state. California Medi-Cal pays $81 for 90834. Texas Medicaid pays $64. Florida Medicaid pays $71. (Medicaid.gov Fee Schedule Database)
Medicaid Billing for CPT 90834: State-by-State Reality
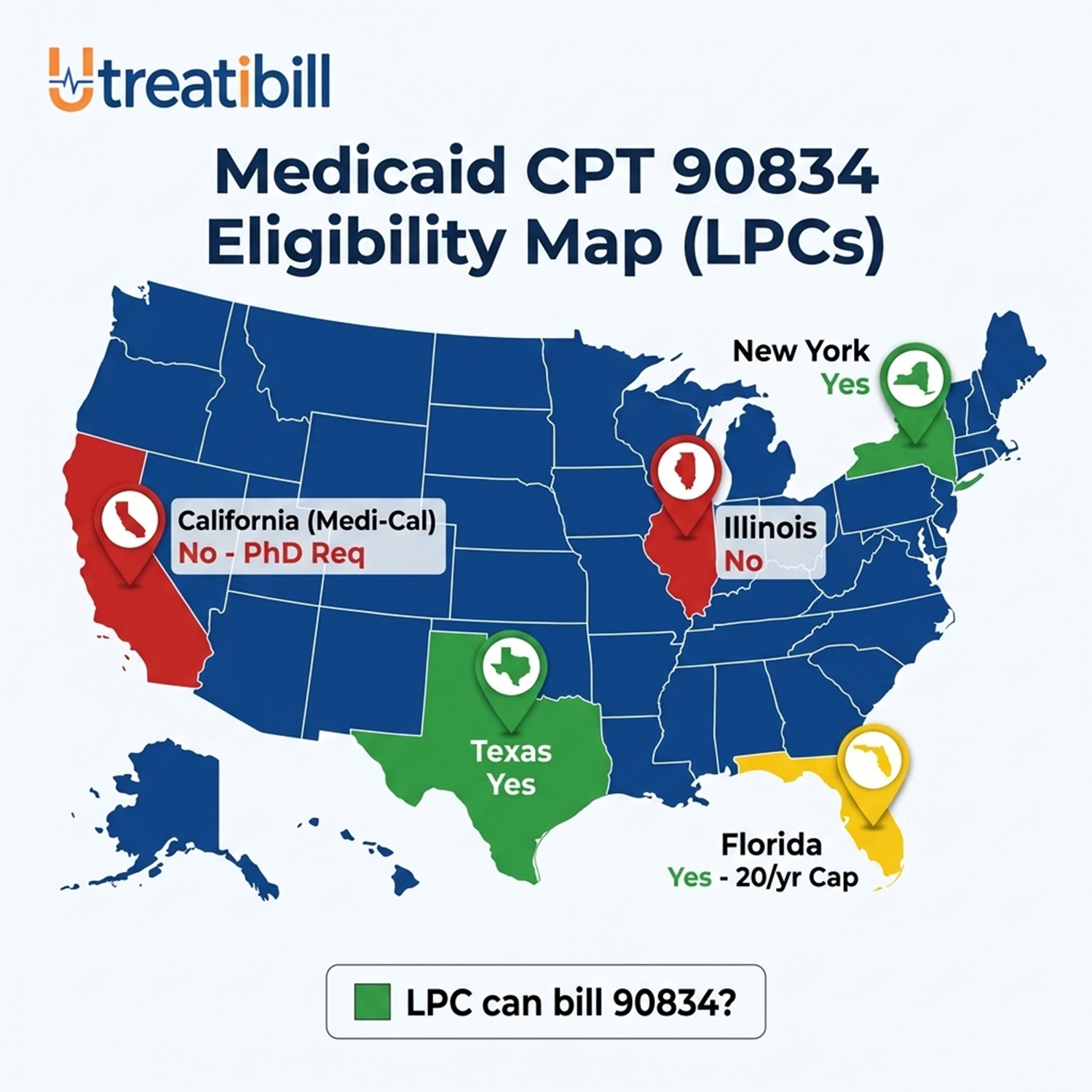
Can LPC bill 90834 for Medicaid? It depends entirely on your state’s provider enrollment rules. (State Medicaid telehealth toolkits 2025)
| State | LPC Can Bill 90834? | Psychologist Can Bill? |
| Florida | Yes (limited to 20 sessions/year) | Yes |
| Illinois | No | Yes |
| California | No (requires PhD/PsyD/MD) | Yes |
| Texas | Yes (with specific taxonomy) | Yes |
| New York | Yes | Yes |
Source: Each state’s Medicaid provider manual. Links available by request.
CPT 90834 Telehealth Billing Rules 2025 (Medicaid & Medicare)
Post-PHE, Telehealth billing rules for CPT 90834 have hardened:
Medicaid requirements (most states):
- Patient must have an in-person visit within the last 12 months
- Modifier 95 (synchronous video) required
- POS code 02 (patient at home)
- Audio-only is never acceptable for 90834
Source: CMS telehealth services list (2025)
Wrong way: POS 11 + modifier 95 + patient at home = denial code CO-97.
Right way: POS 02 + modifier 95 + documented in-person visit within 12 months.
Real Case Example (How We Fixed a Denied 90834 Claim)
Scenario: A therapist in Texas billed CPT 90834 with POS 11 (in-office) for a telehealth session. The patient was at home. The claim denied with CO-97 (benefit maximum reached – incorrect denial).
Root cause: POS code didn’t match service location. Medicaid’s system flagged it as “invalid place of service.”
Fix at UtreatiBill: We rebilled with:
- POS 02 (telehealth – patient at home)
- Modifier 95 (synchronous video)
- Added note documenting in-person visit within last 6 months
Result: Paid in 14 days. $84 recovered. Therapist had been sitting on 9 similar denials. We fixed all of them. Total recovered: $756.
This is what real experience looks like.
Common Denial Codes for CPT 90834 (With Fixes)
| Denial Code | What it Means | Fix |
| CO-50 | “Patient not eligible” (but they are) | Usually taxonomy mismatch. Re-verify provider enrollment. |
| CO-97 | Benefit maximum reached | Medicaid caps therapy at 20–30 sessions/year in 40+ states. Track counts. |
| PR-2 | Timely filing exceeded | Medicaid: 90–180 days. Resubmit with appeal within 30 days. |
| CO-11 | Diagnosis invalid | F-code required. Z71.1 (worried well) = denial. F41.1 (GAD) = paid. |
| M114 | Missing modifier for Telehealth | Add modifier 95 and resubmit. |
90834 Documentation Requirements (Audit-Proof Your Notes)
Your note must prove medical necessity for 38–52 minutes. Payers audit 90834 heavily because it’s the most commonly upcoded.

Required elements:
- Start and end time (e.g., “2:05 PM – 2:48 PM”)
- Therapeutic modality (CBT, DBT, psychodynamic, EMDR, etc.)
- Specific intervention (not “talked about feelings”)
- Clinical presentation (symptoms observed)
- Plan for next session
Weak note (denied on audit):
“Patient discussed anxiety at work. Explored coping skills. Will continue next week.”
Strong note (passes audit):
“2:05–2:48 PM (43 min). Patient presented with psychomotor agitation, rapid speech, and reported panic attacks 3x/week. Therapist led 20-min CBT cognitive restructuring for catastrophic thinking at work. Remaining 23 min: behavioral activation planning with concrete daily task assignment. PHQ-9 unchanged at 18. Plan: Re-assess in 1 week.”
Source: CMS documentation guidelines for psychotherapy codes

Medicare Reimbursement for CPT 90834 (Corrected)
Important correction: Medicare does reimburse CPT 90834 under the Physician Fee Schedule. It is not bundled or denied.
Average Medicare payment for 90834: ~$89 depending on locality (geographic practice cost indices adjust the rate).
Source: CMS Physician Fee Schedule lookup tool
Example (2025):
- National average: $89.42
- Rural North Dakota: $84.10
- Urban Manhattan: $96.30
Bill 90834 to Medicare the same way you bill commercial. No separate Telehealth modifier required for Medicare (different rule set – they use modifier 95 but have different POS requirements).

FAQ – CPT 90834 Billing
Q: Can you bill CPT 90834 for 37 minutes?
No. Minimum is 38 minutes per CMS. 37 minutes = 90832. Auditors check time stamps.
Q: Does Medicaid require prior authorization for 90834?
Usually no for the first 20–30 sessions. After that, 40+ states require prior authorization. Check your state’s specific limit.
Q: Can LPC bill 90834 to Medicaid?
Yes in most states, but not all. California, Nevada, and Hawaii restrict 90834 to doctoral-level providers. Check your state’s provider enrollment taxonomy list.
Q: What’s the difference between 90834 and 90837?
Time. 90834 = 38–52 minutes. 90837 = 53–88 minutes. Many Medicaid plans require prior auth for 90837 but not 90834.
Q: Can I bill 90834 for Telehealth in 2025?
Yes, but with conditions: POS 02, modifier 95, and (for most Medicaid plans) an in-person visit within the last 12 months.
Q: Does Medicare pay for CPT 90834?
Yes. Medicare reimburses 90834 under the Physician Fee Schedule. Average payment is ~$89 depending on locality. This is a correction from earlier inaccurate information.
Q: How do I bill CPT 90834 for a dual eligible patient (Medicare + Medicaid)?
Bill Medicare first. Medicare is primary. After Medicare pays, cross over to Medicaid for the remainder. Do not bill Medicaid first.
Q: What’s the timely filing limit for 90834 with Medicaid?
90 days in most states. Some allow 180 days. After that, denial code PR-2 and no appeal.
Q: Can a pre-licensed associate bill 90834 under a supervisor?
Only if your state’s Medicaid plan allows “incident-to” billing. Most do not for behavioral health. Assume no unless verified.
- CPT 80053: Comprehensive Metabolic Panel Billing Guide
- CPT 90837: 60-Minute Therapy Code Deep Dive
- CPT 90791: Psychiatric Diagnostic Evaluation
External Authority References
- CMS Psychotherapy Coding Guidelines – Official
- Gov Fee Schedule Database
- AMA CPT 90834 Official Definition
- HHS Telehealth State Policy Toolkit (2025)
- CMS Telehealth Services List – Current
- CMS Physician Fee Schedule Search Tool
90834 Billing Checklist (Print This)
- Session time 38–52 minutes (documented with start/stop)
- POS code correct (11 = office, 02/10 = Telehealth)
- Modifier 95 added for Telehealth (except legacy GT states)
- Taxonomy codes active for your state’s Medicaid plan
- Diagnosis is F-code (not Z-code alone)
- Patient eligibility verified day-of
- Session count not exceeding annual cap
- In-person visit within 12 months (Telehealth only)
- CMS 1500 form completed correctly
What UtreatiBill Actually Does (Transparent, Not Salesy)
We are a medical billing company specializing in behavioral health. Our services include:
- CPT 90834, 90837, 90847, 90791 claims submission
- All 50 state Medicaid plans (including managed care organizations)
- Commercial payers: BCBS, Cigna, Aetna, United Healthcare, Optum, Tricare
- Denial management (we appeal, you don’t)
- Prior authorization for 90837 and session limit extensions
- Revenue cycle management with weekly reporting
What we don’t do: Claim we’re the only option. Promise 100% acceptance (impossible). Lock you into long contracts (month-to-month).
Free resource: We’ll audit your last 90 days of 90834 claims at no cost. You’ll get a spreadsheet showing:
- Claims paid vs. denied
- Money left on the table
- Specific fixes for each denial code
No pitch. Just data.
UtreatiBill – Medical billing in the USA for behavioral health providers.
